Custom Billing and Coding Rules Built for You!
Transfer your knowledge into custom-built rules to address your payer requirements, specialties, value-based contracts, and more. Ensure the cleanest claims go out—every time.
Unprecedented Customization
- Gain more control by creating your own custom rules—no IT needed
- Set key rules to autocorrect routine billing errors
- Free up your team's valuable time to focus on more important issues—all while ensuring compliance and improving revenue

“Now, out of 3,000 tasks a day, we probably have to manually review about 100. Everything else automatically posts. Clean claims go out the first time without the need to review them.”

Get a Demo—See What Rules We Can Customize for You!
Custom Rule Examples
The Challenge
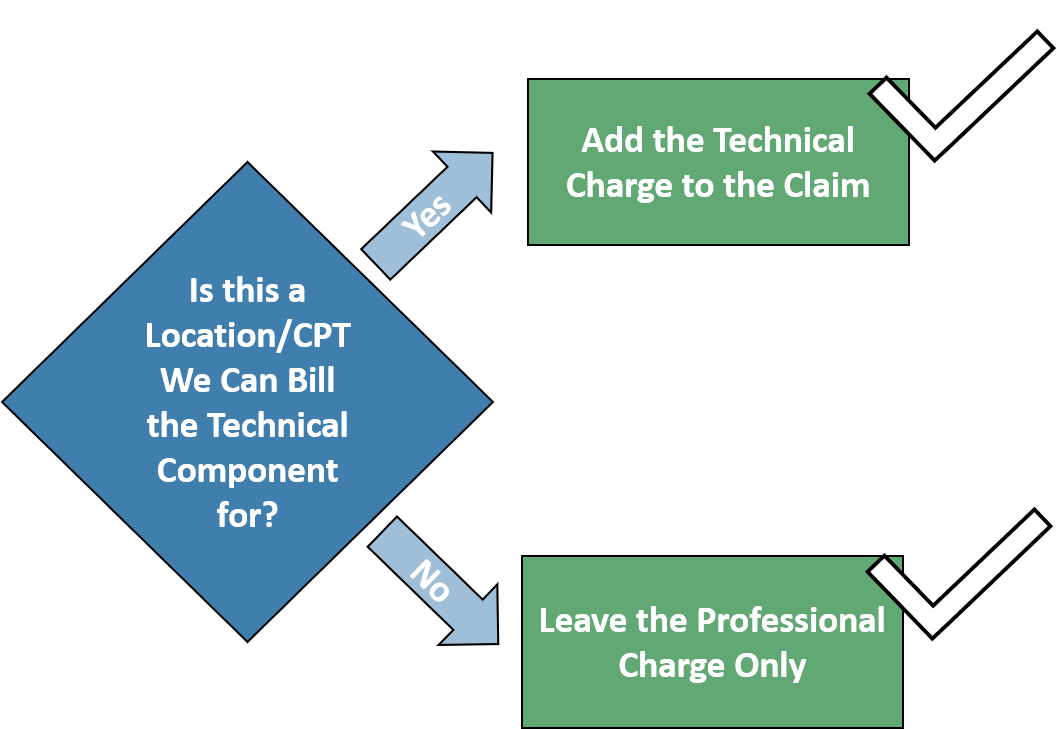
A charge coming from the EMR into the RCM system consists solely of the professional component, but this medical group is able to bill for the technical component as well.
The Solution
A custom rule to automatically add the technical component to a claim. The rule knows which charges require the technical component based on the location and CPT data.
The Challenge
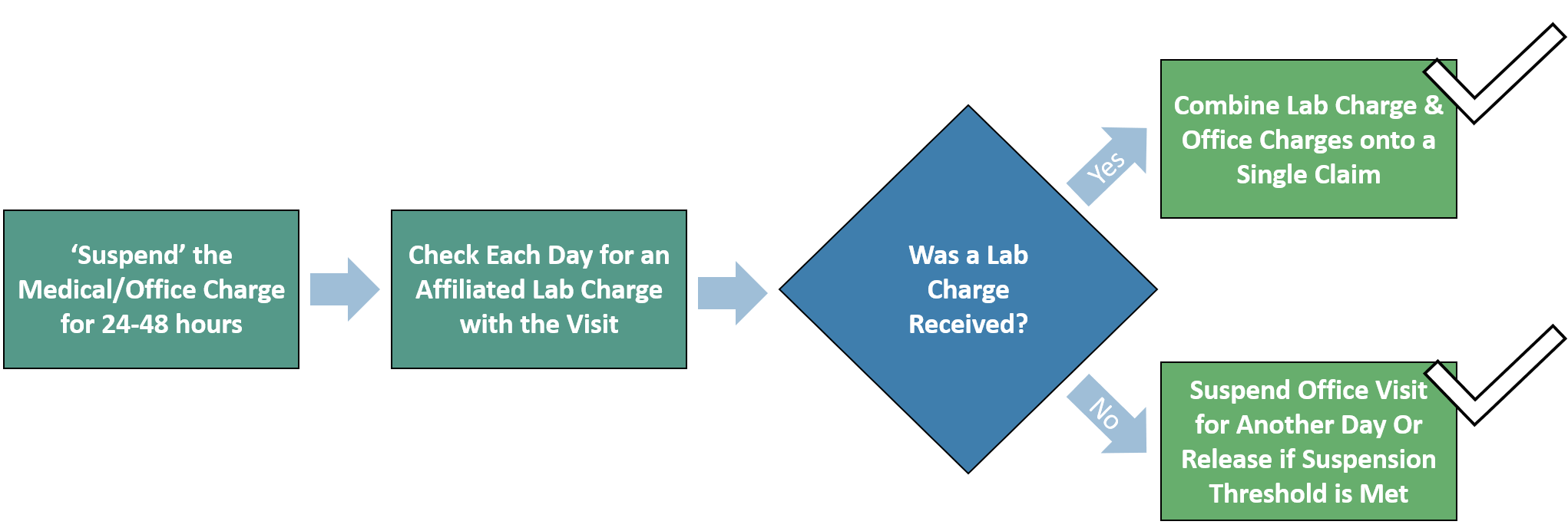
Lab charges affiliated with an office visit are not sent to the RCM system until 24-48 hours after the office visit, but the medical group needs all CPTs included on a single claim.
The Solution
A custom rule to “suspend” office visits for 24-48 hours. Then, every day, check for lab charges affiliated with an office visit and combine all CPTs onto a single claim.
The Challenge
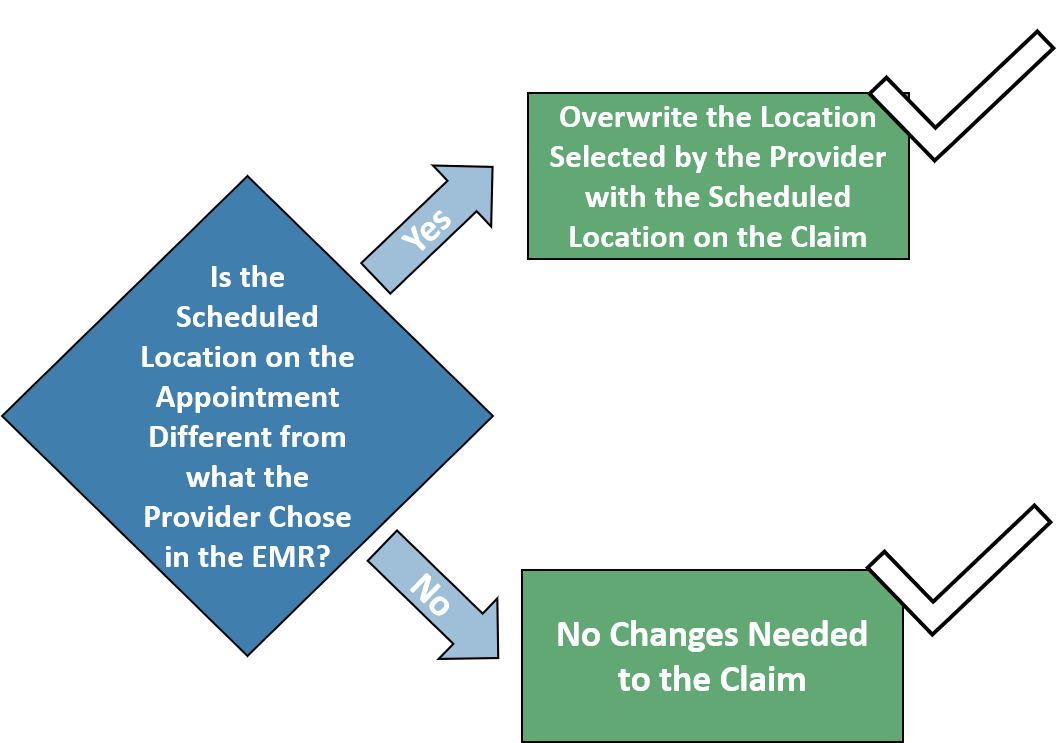
An appointment is scheduled with the accurate location, but the provider chose a different (incorrect) location in the EMR during the visit.
The Solution
A custom rule to compare the appointment data to the charge data and overwrite the incorrect data automatically.
The Challenge
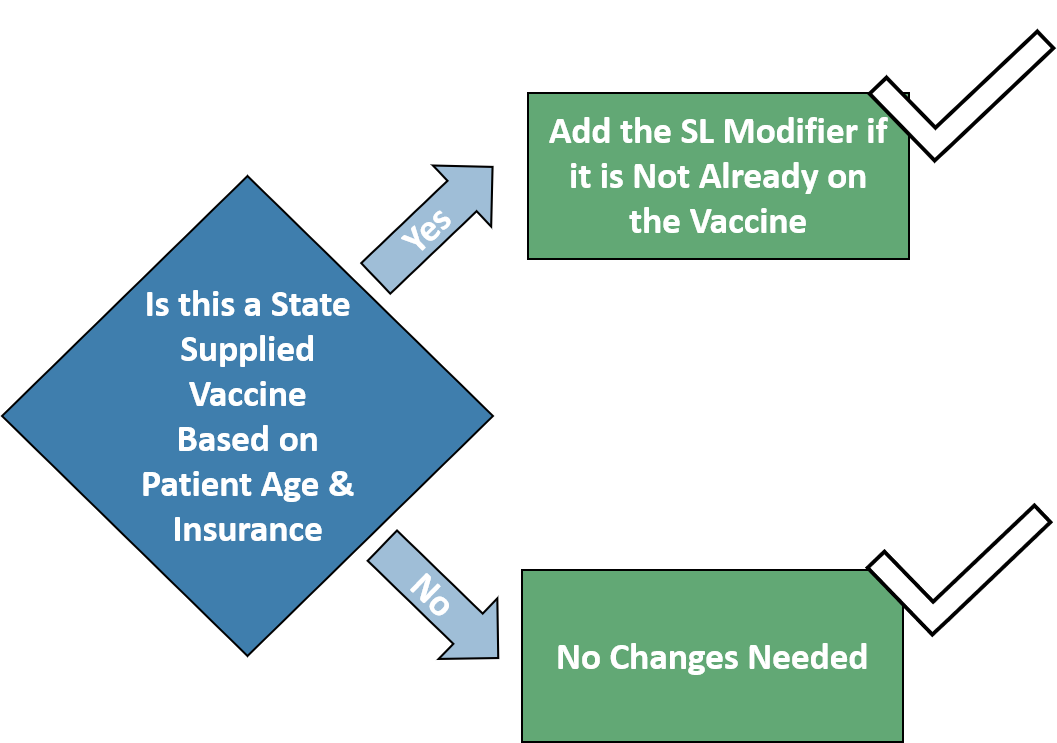
Even though a vaccine is state supplied, the medical group must bill the CPT on a claim and include an SL modifier to denote the vaccine as a $0 charge.
The Solution
Custom rules based on patient age, payer, and vaccine to automatically add the SL modifier when appropriate. Note: Any rule can be automated, so you can automate all administration code billing requirements.
-
The Challenge
A charge coming from the EMR into the RCM system consists solely of the professional component, but this medical group is able to bill for the technical component as well.
The Solution
A custom rule to automatically add the technical component to a claim. The rule knows which charges require the technical component based on the location and CPT data.

-
The Challenge
Lab charges affiliated with an office visit are not sent to the RCM system until 24-48 hours after the office visit, but the medical group needs all CPTs included on a single claim.
The Solution
A custom rule to “suspend” office visits for 24-48 hours. Then, every day, check for lab charges affiliated with an office visit and combine all CPTs onto a single claim.

-
The Challenge
An appointment is scheduled with the accurate location, but the provider chose a different (incorrect) location in the EMR during the visit.
The Solution
A custom rule to compare the appointment data to the charge data and overwrite the incorrect data automatically.

-
The Challenge
Even though a vaccine is state supplied, the medical group must bill the CPT on a claim and include an SL modifier to denote the vaccine as a $0 charge.
The Solution
Custom rules based on patient age, payer, and vaccine to automatically add the SL modifier when appropriate. Note: Any rule can be automated, so you can automate all administration code billing requirements.

Have a complex billing or coding challenge you want to automate?
Frequently Asked Revenue Cycle Rules Questions
-
The RCxRules software uses rules to ensure all charges within a claim are accurate. Each charge is run against a series of rules to ensure the encounter is correct. If a rule is broken, that means the charge did not meet the specific criteria of that rule and needs correcting. Each rule is a piece of logic containing information about industry standards, specialty specifics or other custom information tailored to your organization’s specific needs.
-
While IT can assist with rule writing, the software was built so that your revenue cycle and billing teams can write their own rules. The rule writer utilizes easy-to-understand language and commands to write rules.
-
The rules engine was designed to account for every organization’s most complex issues, which is reflected in the rules engine’s flexibility. For example, a user can write a rule with multiple conditions (payer, provider, place of service, diagnosis code, CPT code, etc.), incorporate translation tables, and account for patient demographic information.
-
No, users may write as many rules as they would like.
-
An autocorrect is a unique capability of the rules engine that automatically fixes routine data issues. A few examples of autocorrect include:
- Automatically adding an administration code to an immunization
- Bundling or unbundling CPT codes based on payer or another requirement
- Automatically adding a modifier based on payer or another requirement
-
RCxRules delivers industry standard rules and high-value, specialty-specific rule sets out of the box. Industry standard rules include CCI, NCD/LCD, MUE, RVU, etc. Most importantly, the RCxRules team will work with you to build rules tailored to your organization’s specific challenges. Then, your team is empowered to build rules as new needs emerge, with RCxRules support standing by ready to assist you if more complex rules are needed.
-
The RCxRules customer base includes most specialties, including primary care, dermatology, pediatrics, lab, radiology, cardiology, orthopedics, urology, anesthesiology, women’s health, CHC/FQHC, nephrology, oncology, and others.
-
The average customer realizes a return that is four times their investment. This ROI is driven by automating the EMR charge review process as well as the automated correction of routine data errors. The rules engine delivers additional value through the reduction of preventable denials, the capture of missed revenue, and acceleration of payer payment.
-
Yes, the rules engine can process charges from an unlimited number of clinical systems such as lab, radiology, mobile charge capture, etc. The rules engine can accept charges in formats such as HL7, Excel, CSV, and Flat File.
-
RCxRules has two integration approaches. The RCxRules software can integrate with your EMR and revenue cycle management systems with standard HL7 interfaces, or it can more deeply integrate with these systems via web services if your systems support it. In both cases, RCxRules replicates critical information from these systems into our rules engine (payer, provider, place of service, CPT, ICD-10, etc.) to seamlessly and accurately process charges.
-
RCxRules has integrated with most major EMR and revenue cycle management systems, including Epic, Cerner, Allscripts, GE, Athena, NextGen as well as many others. Contact us to hear more about how we can integrate with your systems.
.jpeg)