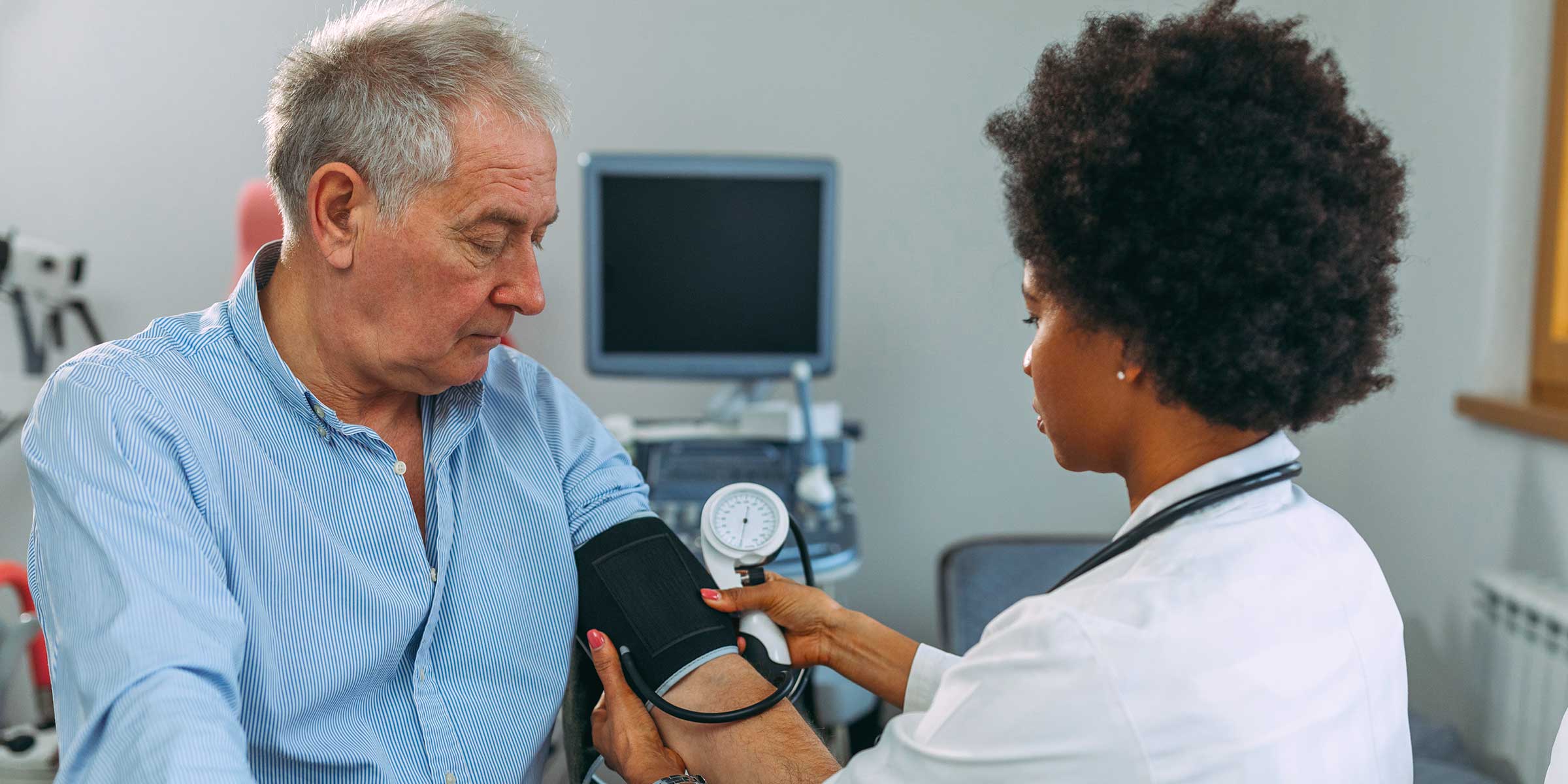
Technology that Helps You Work Smarter
For Revenue Cycle Management and Population Health Teams
Free up your team to spend more time on revenue-boosting work by eliminating unnecessary manual tasks. Our AI-driven solutions will simplify your revenue cycle and risk adjustment workflows by tapping into the time-saving power of automation.
Trusted by





















Solutions that Work for Your Practice
Empower your team to generate more revenue—with less effort. Our software works on the front end of your process, automatically reviewing 100% of charges against revenue cycle and HCC coding rules tailored to your specific needs. Our technology delivers the most accurate and complete billing, coding, and HCC data.
Think of Us as Your Productivity Partner
43,000
providers depend on RCxRules for their automation needs
1.5 million
hours of staff work automated annually
180 million
claims automatically reviewed annually
"The RCxRules software has automated several manual processes such as reducing provider's time in the EHR and charge posting errors. The ease of customizing the software and the high-touch implementation led to a smooth go-live and set the stage for continued success."

Terry Keeling
University Hospitals






.jpeg)