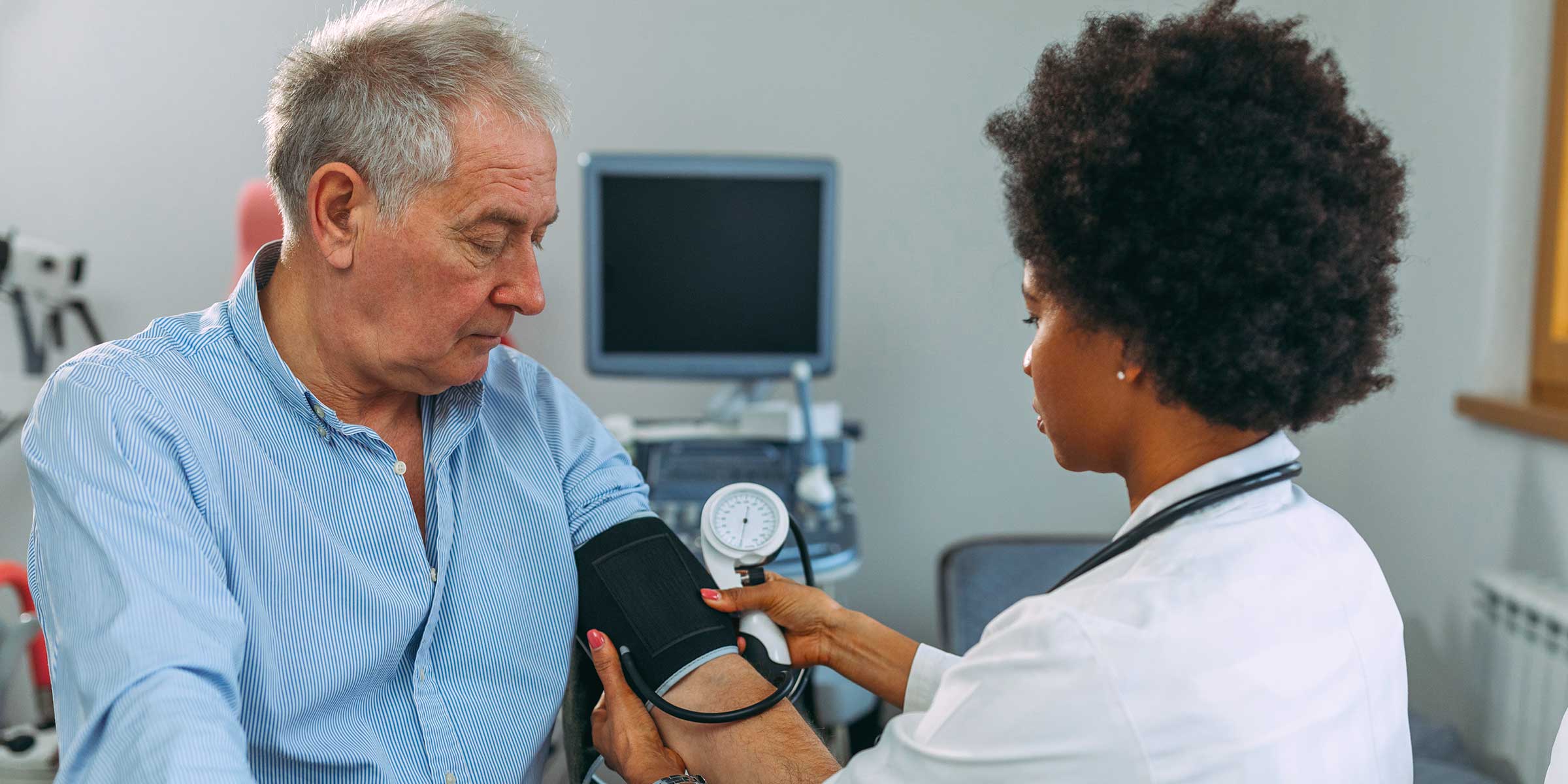
Simplify Your Revenue Cycle Workflow
Every day, you are responsible for processing thousands of charges and ensuring they are turned into clean, payment-ready claims. Since the providers entering these charges went to medical school to become doctors, not coders, you end up with a constant flow of bad data from your clinical systems that requires time and energy to manage. But there is a better way. By turning your unique knowledge and expertise into highly tailored, automated rules that autocorrect billing and coding errors, we create a dramatically more efficient workflow. It’s time to take control of the information and the process, and free up your team to focus on only the most important issues.
Trusted by




















Why Choose the Revenue Cycle Engine?
Our AI-assisted technology integrates with systems you already use. Working seamlessly on the front end of your process, RCxRules reviews each and every charge for coding completeness and accuracy immediately after it leaves your EMR, before a claim is created.
“Now out of 3,000 tasks a day, we probably have to manually review about 100. Everything else automatically posts. Clean claims go out the first time without the need to review them.”

Customization and Control
You and your team are already experts at navigating the complex world of revenue cycle management. We’ll work with you to identify critical areas where custom rules can dramatically reduce the burden of manual effort by automatically correcting routine billing errors.

Fix Bad Data Up Front
The prevalence of EMRs has led to a daily onslaught of bad electronic billing data. Since providers didn’t go to medical school to become coders, you end up with a lot of errors to sort through. And while you didn’t create this system, you are responsible for managing it. RCxRules is here to help–cleaning data at the beginning of the process, saving you countless hours of manual work.

Build a Knowledge Base
Multiple spreadsheets, sticky notes on someone’s desk—chances are your hard-earned institutional knowledge is scattered across your organization. RCxRules gives you one location to host your organization’s billing and coding knowledge. This centralized knowledge base allows you to keep up with ever-evolving payer requirements and make sure everyone on your team handles billing and coding issues exactly as instructed for every encounter—as if you were personally sitting next to each one of them as they work.

Optimize Staffing
Historically, the charge review process required extensive and expensive staffing. With RCxRules, that outdated approach is a thing of the past. RCxRules identifies only those charges that require manual review, so your team can focus their efforts where they’re needed most. Simply put: hire technology, not more people.

-
Fix Bad Data Up Front
The prevalence of EMRs has led to a daily onslaught of bad electronic billing data. Since providers didn’t go to medical school to become coders, you end up with a lot of errors to sort through. And while you didn’t create this system, you are responsible for managing it. RCxRules is here to help–cleaning data at the beginning of the process, saving you countless hours of manual work.

-
Build a Knowledge Base
Multiple spreadsheets, sticky notes on someone’s desk—chances are your hard-earned institutional knowledge is scattered across your organization. RCxRules gives you one location to host your organization’s billing and coding knowledge. This centralized knowledge base allows you to keep up with ever-evolving payer requirements and make sure everyone on your team handles billing and coding issues exactly as instructed for every encounter—as if you were personally sitting next to each one of them as they work.

-
Optimize Staffing
Historically, the charge review process required extensive and expensive staffing. With RCxRules, that outdated approach is a thing of the past. RCxRules identifies only those charges that require manual review, so your team can focus their efforts where they’re needed most. Simply put: hire technology, not more people.

How the Revenue Cycle Engine Benefits Your Organization
CFOs
Hit your financial targets through reliable, predictable, and surprise-free revenue generation. Automatically identify potential missed charges to streamline operations and establish a proven and demonstrable ROI.
Revenue Cycle Management Leaders
Ensure a 100% consistent application of standard billing procedures across your entire team. Free up your staff from time-consuming routine issues to focus on critical, revenue-generating activities. Reduce costly staff overtime and minimize the stressful month-end crunch, so your revenue cycle team can be even more productive and happy.
Billing Staff
Eliminate the need to fix routine billing problems over and over so you can focus on only the most important issues. Work smarter with the fast, efficient, and user-friendly task management and charge edit interface that was built by revenue cycle experts for revenue cycle experts.
.jpeg)