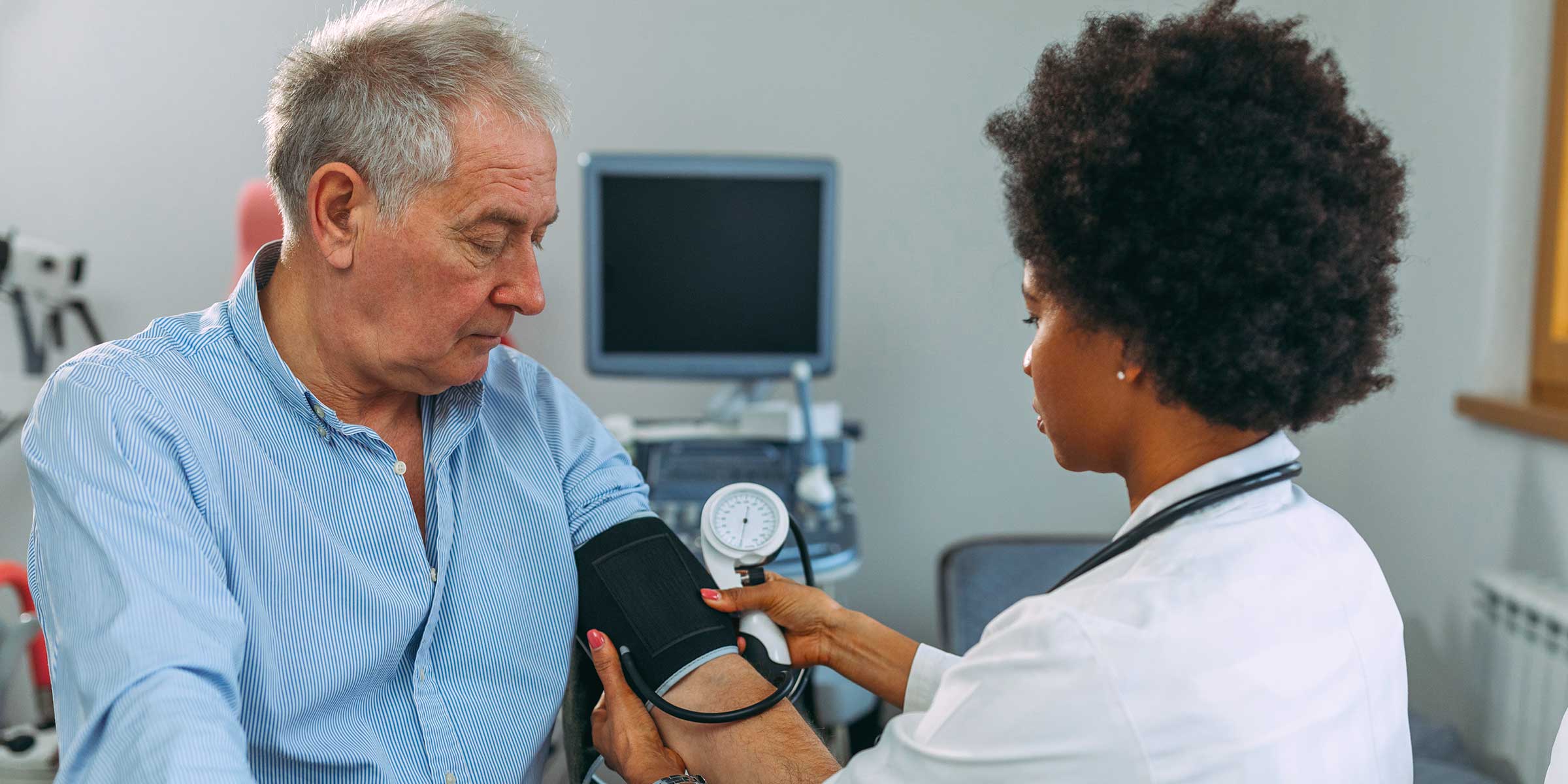
Urology Medical Billing Software
The Revenue Cycle Engine
Boost your revenue and improve staff efficiency with highly tailored, automated rules that optimize your urology revenue cycle management.
“We are big advocates of RCxRules and consider it to be one of the best technological investments we have made. It is one of those rare instances where the product turned out to be even more powerful than we had been anticipating during the sales process.”
Get a Demo of Our Urology Medical Billing Software.
Trusted By





























Customization and Control
You and your team are already experts at navigating the complex world of urology revenue cycle management. We’ll work with you to identify critical areas where custom rules can dramatically reduce the burden of manual effort by automatically correcting routine billing errors.
Custom Urology Rule Examples
The Challenge
Medicare does not allow ultrasound procedure code 76942 With 76872.
The Solution
When billing Medicare for procedure code 76872 (ultrasound, transrectal), this rule automatically removes procedure code 76942 (ultrasonic guidance for needle placement).

The Challenge
Urethrocystography and cystography procedures require an additional injection procedure code.
The Solution
When billing procedure code 74455 (urethrocystography), or 74430 (cystography), this rule automatically adds procedure code 51600 (injection procedure for cystography or voiding urethrocystography), if missing, to the encounter.

The Challenge
Temporary ureteral catheter should not be billed separately when cystourethroscopy or pyeloscopy are performed.
The Solution
When billing diagnostic or therapeutic cystourethroscopy with ureteroscopy and/or pyeloscopy using procedure codes 52320-52356, the insertion and removal of a temporary ureteral catheter procedure code 52005 is included and should not be billed separately. This rule automatically removes procedure code 52005.

The Challenge
The diagnosis is side-specific (affecting the right or left kidney) and needs a laterality modifier.
The Solution
When billing with a diagnosis code that specifies left side or right side, this rule automatically adds the appropriate LT or RT modifier.

-
The Challenge
Medicare does not allow ultrasound procedure code 76942 With 76872.
The Solution
When billing Medicare for procedure code 76872 (ultrasound, transrectal), this rule automatically removes procedure code 76942 (ultrasonic guidance for needle placement).

-
The Challenge
Urethrocystography and cystography procedures require an additional injection procedure code.
The Solution
When billing procedure code 74455 (urethrocystography), or 74430 (cystography), this rule automatically adds procedure code 51600 (injection procedure for cystography or voiding urethrocystography), if missing, to the encounter.

-
The Challenge
Temporary ureteral catheter should not be billed separately when cystourethroscopy or pyeloscopy are performed.
The Solution
When billing diagnostic or therapeutic cystourethroscopy with ureteroscopy and/or pyeloscopy using procedure codes 52320-52356, the insertion and removal of a temporary ureteral catheter procedure code 52005 is included and should not be billed separately. This rule automatically removes procedure code 52005.

-
The Challenge
The diagnosis is side-specific (affecting the right or left kidney) and needs a laterality modifier.
The Solution
When billing with a diagnosis code that specifies left side or right side, this rule automatically adds the appropriate LT or RT modifier.

Have a complex urology billing or coding challenge you want to automate?
Why Choose the Revenue Cycle Engine?
Our technology integrates with systems you already use. Working seamlessly on the front end of your process, RCxRules reviews each and every charge for coding completeness and accuracy immediately after it leaves your EMR, before a claim is created.
“I appreciate RCxRules for their quick responses, commitment to excellence, organization, and exceptional knowledge. They were fantastic to work with. During implementation, when there were unforeseeable bumps, they provided the best support to ensure all of our needs were met beyond expectation.”
Fix Bad Data Up Front
The prevalence of EMRs has led to a daily onslaught of bad electronic billing data. Since providers didn’t go to medical school to become coders, you end up with a lot of errors to sort through. And while you didn’t create this system, you are responsible for managing it. RCxRules is here to help–cleaning data at the beginning of the process, saving you countless hours of manual work.

Build a Knowledge Base
Multiple spreadsheets, sticky notes on someone’s desk—chances are your hard-earned institutional knowledge is scattered across your organization. RCxRules gives you one location to host your organization’s billing and coding knowledge. This centralized knowledge base allows you to keep up with ever-evolving payer requirements and make sure everyone on your team handles billing and coding issues exactly as instructed for every encounter—as if you were personally sitting next to each one of them as they work.

Optimize Staffing
Historically, the charge review process required extensive and expensive staffing. With RCxRules, that outdated approach is a thing of the past. RCxRules identifies only those charges that require manual review, so your team can focus their efforts where they’re needed most. Simply put: hire technology, not more people.

-
Fix Bad Data Up Front
The prevalence of EMRs has led to a daily onslaught of bad electronic billing data. Since providers didn’t go to medical school to become coders, you end up with a lot of errors to sort through. And while you didn’t create this system, you are responsible for managing it. RCxRules is here to help–cleaning data at the beginning of the process, saving you countless hours of manual work.

-
Build a Knowledge Base
Multiple spreadsheets, sticky notes on someone’s desk—chances are your hard-earned institutional knowledge is scattered across your organization. RCxRules gives you one location to host your organization’s billing and coding knowledge. This centralized knowledge base allows you to keep up with ever-evolving payer requirements and make sure everyone on your team handles billing and coding issues exactly as instructed for every encounter—as if you were personally sitting next to each one of them as they work.

-
Optimize Staffing
Historically, the charge review process required extensive and expensive staffing. With RCxRules, that outdated approach is a thing of the past. RCxRules identifies only those charges that require manual review, so your team can focus their efforts where they’re needed most. Simply put: hire technology, not more people.